Obsessive-Compulsive Disorder
Home // Obsessive-Compulsive Disorder
What is Obsessive-Compulsive Disorder?
Obsessive-Compulsive Disorder (OCD) is a mental health condition characterized by recurring, intrusive thoughts (obsessions) and repetitive behaviors or mental acts (compulsions). People with OCD often experience intense anxiety and distress due to their obsessions, which are unwanted and intrusive thoughts, images, or urges that feel uncontrollable. In response to these obsessions, individuals engage in compulsions, which are repetitive behaviors or mental rituals performed to alleviate anxiety or prevent a feared outcome. While engaging in compulsions may provide temporary relief, it ultimately perpetuates the cycle of obsessions and compulsions.
Causes of OCD
- Genetics: OCD tends to run in families, suggesting a genetic component. Certain genes may increase the vulnerability to developing OCD, although no specific genes have been identified as the sole cause.
- Brain abnormalities: There may be differences in the structure and functioning of certain brain areas involved in decision-making, judgment, and behavior regulation in individuals with OCD. The exact nature of these abnormalities is still being studied.
- Chemical imbalance: Imbalances in certain neurotransmitters, particularly serotonin, are thought to play a role in the development of OCD. Serotonin is involved in regulating mood, anxiety, and behavior.
- Environmental factors: Stressful life events, such as trauma, abuse, or significant life changes, can trigger or exacerbate OCD symptoms in individuals who are already predisposed to the disorder. However, not everyone with OCD has experienced a specific traumatic event.
- Cognitive factors: Certain patterns of thinking and cognitive processes may contribute to the development and maintenance of OCD. For example, individuals with OCD may have a heightened sense of responsibility, excessive need for certainty, or difficulty tolerating uncertainty.
Symptoms of Obsessive-Compulsive Disorder

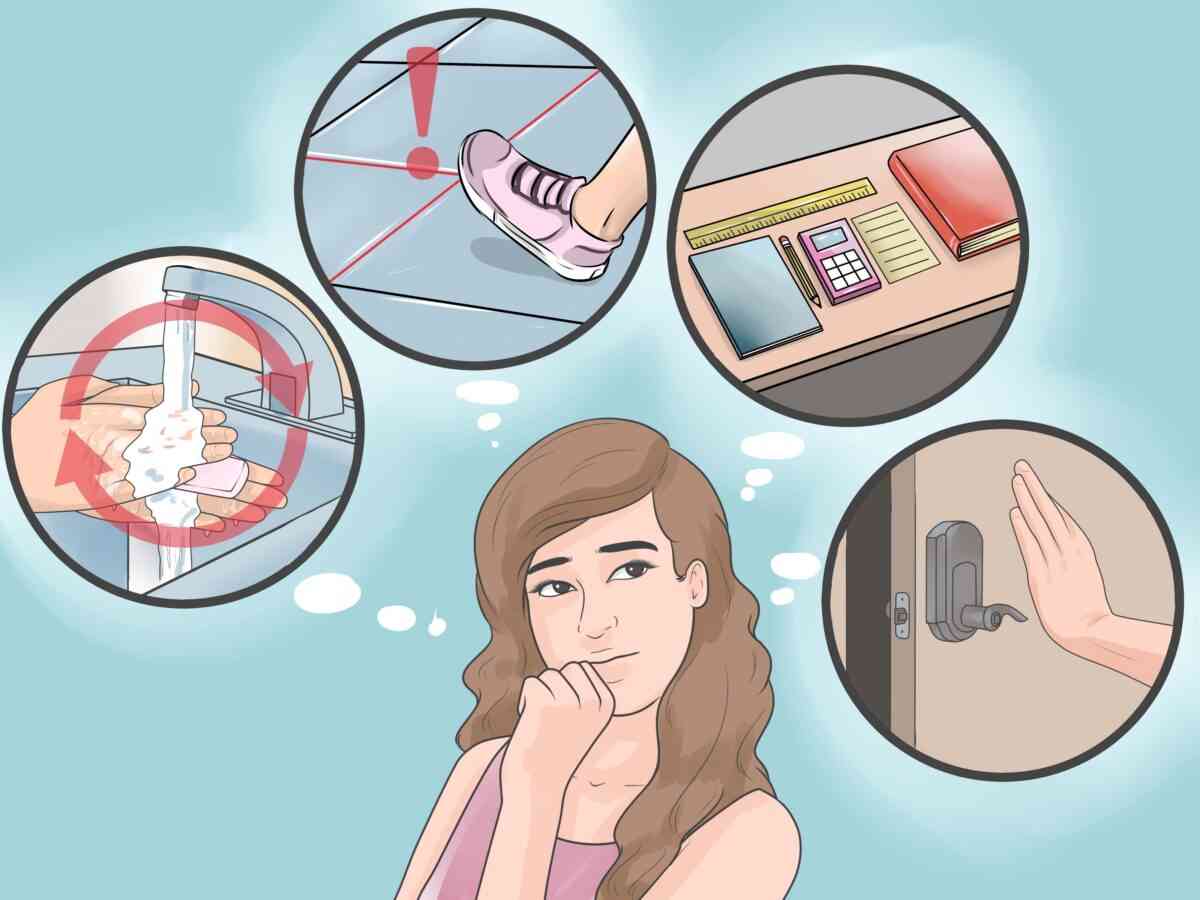
Obsessions
- Fear of contamination or dirt.
- Unwanted, intrusive thoughts about harm, violence, or aggression.
- Excessive concern with order, symmetry, or exactness.
- Unpleasant sexual or religious thoughts.
- Fear of making a mistake or being responsible for something terrible happening.
Compulsions
- Excessive handwashing, cleaning, or sanitizing.
- Repeatedly checking things (e.g., locks, appliances) to prevent harm.
- Counting, repeating words or phrases silently, or performing rituals to reduce anxiety.
- Need for symmetry or arranging items in a particular way.
Hoarding or collecting unnecessary items.
Emotional and Behavioral Symptoms
- High levels of anxiety or distress due to obsessions.
- Feeling a strong urge to perform compulsive behaviors.
- Spending significant time (an hour or more each day) on obsessions and compulsions, which can interfere with daily activities.
- Attempting to resist engaging in compulsions, but experiencing significant distress if unable to perform them.
- Recognizing that the obsessions and compulsions are excessive or unreasonable, but feeling unable to stop them.
Treatments of OCD
Obsessive-compulsive disorder (OCD) is a mental health condition characterized by recurring intrusive thoughts (obsessions) and repetitive behaviors (compulsions). While there is no known cure for OCD, there are various treatment options available that can help manage the symptoms and improve the quality of life. Here are some commonly used treatments for OCD:
- Cognitive-Behavioral Therapy (CBT): CBT is the most effective form of psychotherapy for OCD. It involves two main components: exposure and response prevention (ERP) and cognitive therapy. ERP exposes individuals to situations that trigger their obsessions while preventing the accompanying compulsive behaviors. Over time, this helps reduce the anxiety associated with the obsessions.
- Medication: Selective serotonin reuptake inhibitors (SSRIs) are often prescribed as the first-line medication treatment for OCD. These medications, such as fluoxetine (Prozac), sertraline (Zoloft), and fluvoxamine (Luvox), help to regulate serotonin levels in the brain and can reduce the severity of symptoms.
- Augmentation Strategies: Sometimes, if SSRIs alone are not sufficient, other medications like antipsychotics or mood stabilizers can be added to enhance the effects of treatment. This is known as augmentation.
- Mindfulness-Based Therapies: Mindfulness techniques, such as mindfulness-based cognitive therapy (MBCT) and acceptance and commitment therapy (ACT), can help individuals develop skills to accept their obsessions and reduce their efforts to control or eliminate them. These approaches focus on increasing awareness and acceptance of thoughts and feelings without judgment.
- Support Groups: Participating in support groups or joining OCD-specific communities can provide individuals with a sense of belonging and understanding. Sharing experiences and receiving support from others who have similar struggles can be helpful in managing OCD symptoms.
- Self-Help Strategies: There are several self-help strategies that individuals with OCD can practice alongside therapy. These may include stress management techniques, regular exercise, maintaining a healthy lifestyle, and practicing relaxation exercises.
It’s important to note that the treatment approach may vary depending on the individual and the severity of their symptoms. It is recommended to consult with a mental health professional who specializes in OCD for a proper diagnosis and personalized treatment plan.
