Borderline Personality Disorder
Home // Borderline Personality Disorder
What is Borderline Personality Disorder?
Borderline Personality Disorder (BPD) is a mental health condition characterized by pervasive instability in mood, self-image, behavior, and interpersonal relationships. Individuals with BPD often experience intense emotions, impulsivity, and a fear of abandonment. They may exhibit patterns of unstable and turbulent relationships, have difficulty regulating their emotions, and engage in self-destructive behaviors such as self-harm or suicidal tendencies. BPD can significantly impact a person’s daily functioning and overall quality of life. Treatment typically involves a combination of psychotherapy, medication, and support from mental health professionals.

Causes for (BPD)
- Genetic Factors: Research suggests that there may be a genetic predisposition to developing BPD. Studies have shown that individuals with a family history of BPD or other mood disorders are at a higher risk of developing the disorder themselves. However, specific genes related to BPD have not been identified.
- Environmental Factors: Adverse childhood experiences, such as physical or sexual abuse, neglect, or unstable family environments, have been associated with the development of BPD. Other environmental factors, such as early parental loss or trauma, can also contribute to the risk of developing the disorder.
- Neurobiological Factors: Brain abnormalities and dysfunctions in certain neurotransmitter systems have been observed in individuals with BPD. Research has shown that there may be alterations in the areas of the brain that regulate emotions, impulse control, and decision-making.
- Emotional Sensitivity and Reactivity: Individuals with BPD tend to have heightened emotional sensitivity and reactivity. They may experience intense emotional responses to everyday situations and struggle with regulating their emotions effectively.
- Invalidating Environments: Growing up in an environment where emotions are consistently invalidated or dismissed can contribute to the development of BPD. This can result in individuals having difficulty understanding and regulating their own emotions and seeking external validation.
- Co-occurring Mental Health Conditions: BPD commonly co-occurs with other mental health disorders, such as depression, anxiety disorders, substance use disorders, and eating disorders. The presence of these conditions can complicate the diagnosis and treatment of BPD.
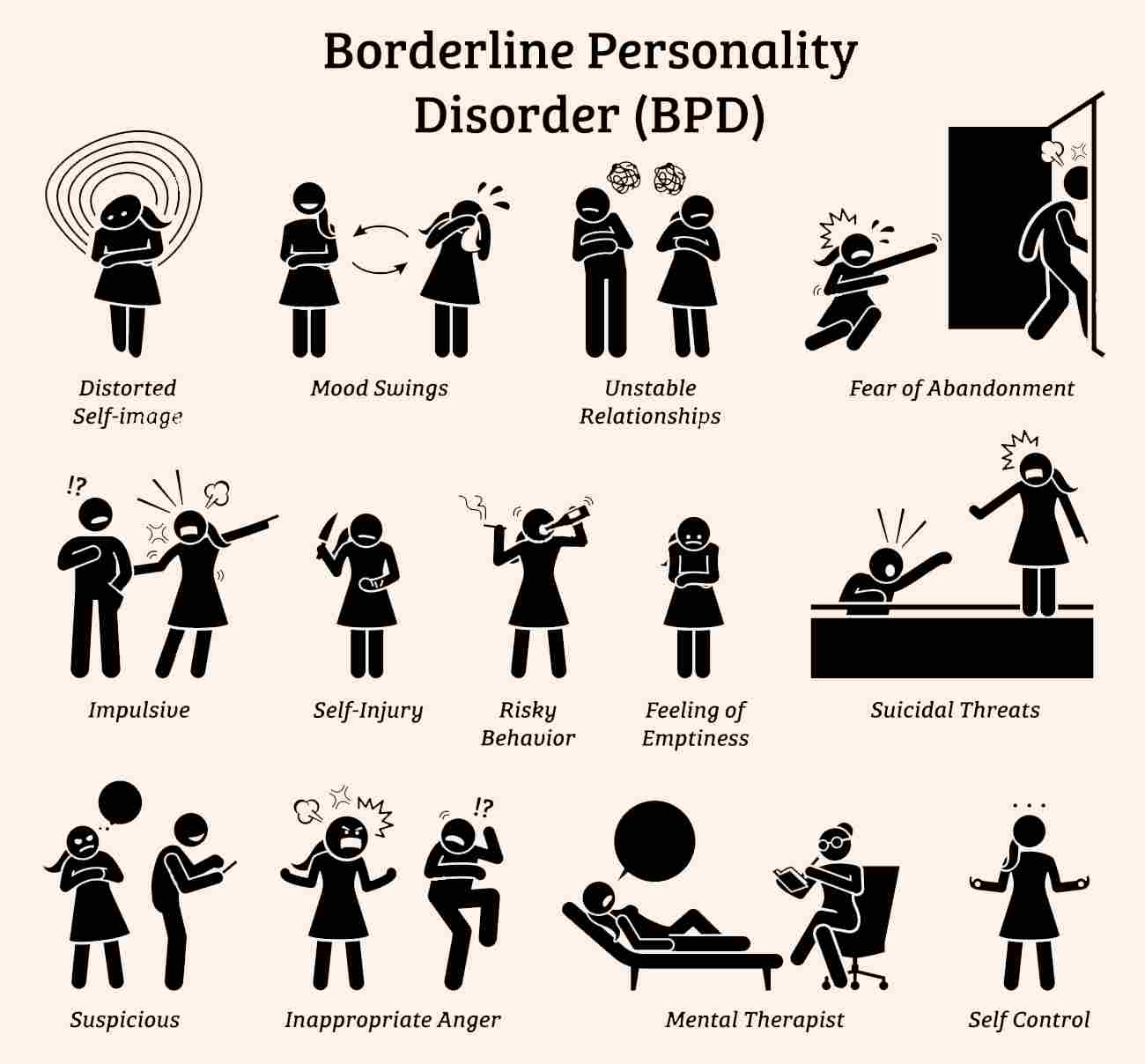
Symptoms of Borderline Personality Disorder
- Intense and unstable relationships
- Emotional instability
- Impulsive behaviors
- Distorted self-image
- Fear of abandonment
- Chronic feelings of emptiness
- Self-harm and suicidal tendencies
- Dissociation
Treatments for (BPD)
Borderline Personality Disorder (BPD) is a complex mental health condition that requires a comprehensive treatment approach. It is important to note that I am an AI language model and not a mental health professional, but I can provide you with some general information on the treatment options commonly used for BPD. It is always recommended to consult with a qualified healthcare provider for an accurate diagnosis and personalized treatment plan. Here are some common approaches to BPD treatment:
- Psychotherapy: Psychotherapy, particularly Dialectical Behavior Therapy (DBT), is often considered the treatment of choice for BPD. DBT focuses on enhancing coping skills, emotional regulation, mindfulness, and interpersonal effectiveness. Other types of therapy, such as cognitive-behavioral therapy (CBT), schema-focused therapy, and psychodynamic therapy, may also be beneficial.
- Medication: While there is no specific medication approved for BPD, certain medications may be prescribed to address specific symptoms or co-occurring conditions. For example, antidepressants, mood stabilizers, and antipsychotic medications might be prescribed to target depression, mood swings, anxiety, or psychotic symptoms if present. Medication is typically used in conjunction with psychotherapy.
- Group therapy: Participating in group therapy or support groups can be helpful for individuals with BPD. Group settings provide opportunities to learn from others, improve social skills, and reduce feelings of isolation. It allows individuals to receive support and understanding from peers who may share similar experiences.
- Hospitalization or intensive treatment programs: In some cases, individuals with BPD may require hospitalization or intensive treatment programs, especially during times of crisis or when self-harm or suicidal ideation is present. These programs offer a structured and intensive therapeutic environment to stabilize individuals and provide ongoing treatment.
- Self-help strategies: Self-help strategies can complement formal treatment. Examples include practicing self-care, engaging in activities that promote relaxation and well-being, developing healthy coping mechanisms, and seeking out educational resources or literature on BPD.
It’s important to remember that treatment for BPD is highly individualized, and what works for one person may not work for another. It often requires a combination of different approaches tailored to the individual’s needs. Consulting with a mental health professional is crucial for an accurate diagnosis and to develop an appropriate treatment plan.
Useful link
Contact
- 2310 N henderson ave Dallas, Texas 75206.
- 1801 e camelback rd ste 102 Phoenix, Arizona 85016.
Copyright © 2026 Psychiatry
